Fossil Focus: Oviraptorosauria
by Waisum Ma
Introduction:
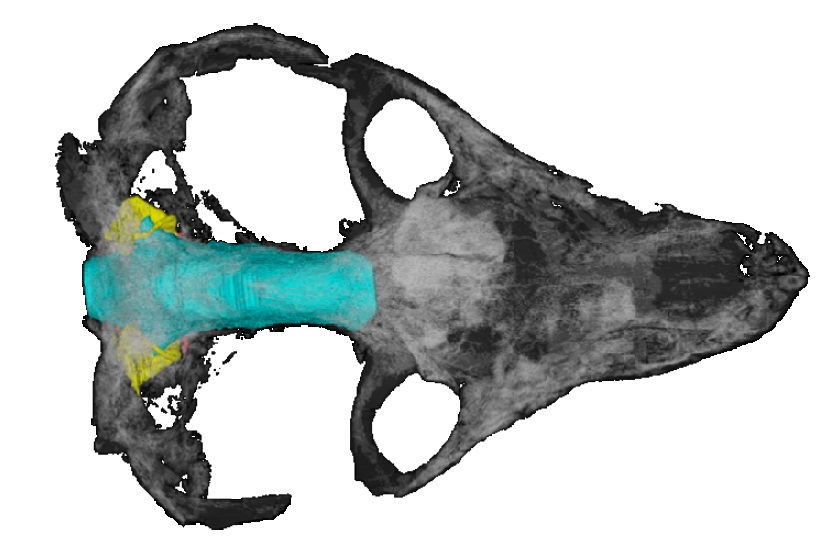
Oviraptorosauria is a group of theropod dinosaurs that first appeared around 125 million years ago, during the early Cretaceous period. They evolved into diverse forms before being wiped out 66 million years ago in the extinction at the end of the Cretaceous, an event that killed all the non-avian dinosaurs. The first known oviraptorosaurian — called Oviraptor — was unearthed in 1923 by the American Museum of Natural History expedition team in the Gobi Desert of Mongolia. It was found near some eggs assumed to be from the dinosaur Protoceratops, which led researchers to infer that Oviraptor stole the eggs of other species — the name means ‘egg thief’. This interpretation was refuted after researchers discovered oviraptorosaurian fossils brooding nests of th...